
The incremental cost-effectiveness ratio (ICER) of NIV + IPI therapy compared with chemotherapy was estimated. Utilities were derived from published sources outside Japan. Cost estimates were based on a Japanese healthcare system perspective using real-world data from the JMDC claims database. Data on overall survival and progression-free survival were derived from the CheckMate 227 trial.
#Checkmate 227 plus
This study aimed to evaluate the cost-effectiveness of combination therapy of nivolumab plus ipilimumab (NIV + IPI) for patients with advanced non-small-cell lung cancer (NSCLC), comparing it with platinum-doublet chemotherapy in Japanese settings.Ī partitioned survival model was developed to predict costs and quality-adjusted life-years (QALYs) in a NIV + IPI arm and a chemotherapy arm.
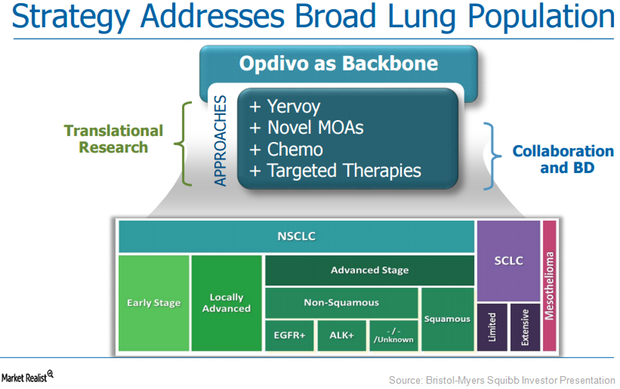
In Japan, indications for nivolumab have been expanded to include the combination therapy with ipilimumab in various cancers. Consistent with findings for all randomized patients, these data support the use of nivolumab plus ipilimumab as first-line treatment of Asian patients with advanced NSCLC. Grade 3-4 treatment-related adverse events occurred in 40% of patients receiving nivolumab plus ipilimumab and 36% receiving chemotherapy, in the overall Asian subpopulation (tumor PD-L1 expression ≥1% and <1%) no new safety signals were identified.Īt 3-year follow-up, nivolumab plus ipilimumab provided durable long-term efficacy benefits versus chemotherapy regardless of tumor PD-L1 expression in the Asian subpopulation, including Japanese patients. Similar results were observed regardless of tumor PD-L1 expression and in Japanese patients. The 3-year progression-free survival rate was 26% versus 7% (HR, 0.65 95% CI 0.45-0.96), objective response rate was 56% versus 37%, and median duration of response was 29.0 months (95% CI 15.0 months-not reached) versus 6.9 months (95% CI 3.9-11.1 months). Median OS was not reached with nivolumab plus ipilimumab versus 24.8 months with chemotherapy 3-year OS rate was 53% versus 37%. In the Asian subpopulation with PD-L1 ≥1%, 81 patients received nivolumab plus ipilimumab and 81 received chemotherapy. Overall survival (OS), progression-free survival, objective response rate, duration of response, and safety were evaluated among patients in Japan, South Korea, and Taiwan. Patients with stage IV/recurrent NSCLC were randomized 1 : 1 : 1 to nivolumab plus ipilimumab, nivolumab monotherapy, or chemotherapy (PD-L1 ≥1%) or nivolumab plus ipilimumab, nivolumab plus chemotherapy, or chemotherapy (PD-L1 <1%). Here we report efficacy and safety results for the Asian subpopulation. Nivolumab plus ipilimumab demonstrated clinically meaningful improvement in efficacy versus chemotherapy with a manageable safety profile in patients with advanced non-small cell lung cancer (NSCLC) and tumor programmed death-ligand 1 (PD-L1) expression ≥1% or <1% in Part 1 of CheckMate 227.
